Product Types | Indications | Benefits | How to Use | Videos | Case Studies | Brochures | References
Osteoallograft® is the tried and true solution for natural bone healing and the BENCHMARK against which the performance of all other bone graft materials is measured.
Osteoallograft® Periomix®is natural, real bone graft designed specifically for veterinary dentistry. It consists of osteoinductive Demineralized Bone Matrix (DBM) and osteoconductive cancellous bone chips. The demineralization of graft allows for immediate access to the growth factors (BMPs) inherent in allograft bone when it is placed into the surgery site. This results in an early beginning of the healing process and helps to make allograft as effective as autograft.
Using bone allograft in periodontics allows you to:
- Restore periodontium to save teeth instead of extracting them.
- Effectively restore bone in extraction sites and in periodontal pockets to support good oral and systemic health and to prevent fracture of the mandible.
- Achieve faster and stronger bone healing compared with using bone substitutes, because it provides both an osteoconductive scaffold and also osteoinductive growth factors (BMPs).1-5 No other bone graft substitute available on the market provides BOTH critical factors for speedy bone healing.
Product Types
Indications:
Tooth extractions
Furcation defects
Horizontal & vertical bone loss
Fracture of the mandible
Volumes (Freeze-Dried):
0.3 cc
0.5 cc
3.0 cc
Osteoallograft® Periomix® is professional-grade allograft:
- Processed aseptically meeting USP guidelines for sterility and secondarily sterilized with gamma irradiation.
- Acellular and processed by methods that have been shown to reduce immunogenicity making immune reactions not a significant concern and eliminating the need for any type of patient matching
- Our production practices are GMP and Good Tissue Practices compliant and modeled after human tissue banking standards
- Our stringent Quality Assurance Program provides confidence and consistency in our products
Indications
Use Osteoallograft® Periomix® for:
- Tooth extractions
- Furcation defects
- Horizontal and vertical bone loss
- Fracture of the mandible
- Any other void filling or bone augmentation procedure that requires grafting
Veterinarian and Patient Benefits
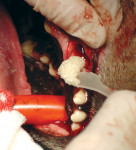
After Extractions:
Applying bone allograft after tooth extractions quickly restores bone in extractions sites.1,6 And due to its osteoinductive growth factors, natural allograft restores bone faster and stronger than bone substitutes.1-5 To see a Comparison Chart with Bioactive Glass, click here.Why restore bone in extraction sites:
- Unfilled extraction sites can harbor bacteria and enable progression of periodontal disease, which in turn can cause further bone and tooth loss and can have systemic effects
- Leaving deep extraction sites unfilled can result in weakened jaw bone or a pathologic fracture
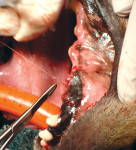
For Tooth Preservation:
Applying bone allograft around exposed roots rapidly restores bone lost due to periodontal disease and results in reconstruction of the attachment apparatus thus preserving teeth. 1,2,6
Why restore the attachment apparatus:
- Allows you to preserve teeth rather than extracting them. Missing teeth result in a lack of stimulation of the underlying bone structure, which can result in bone loss.
- If exposed roots are left untreated, periodontal disease and bone loss will continue
- Bone loss can result in abscess formation, weakened jaw bone, or a pathologic fracture
- Periodontal disease has systemic effects
- Exposed roots are likely to be painful
How to Use
Product Handling Videos
VTS Osteoallograft Periomix Bone Graft in a Maxillary Molar Extraction
VTS Osteoallograft Periomix Bone Graft in a Mandibular Molar Extraction
VTS Osteoallograft Periomix Bone Graft in a Maxillary Canine Extraction
VTS Osteoallograft Periomix Bone Graft Implant Case
VTS Osteoallograft Periomix Bone Graft all 5 cases together
Laboratory on Bone Augmentation Techniques, Dr. Loic Legendre
Informative 6 minute How-To video for canine extractions, oronasal fistula repair, cleft palate repair and fracture mandible repair. Courtesy of Dr. Loic Legendre. This is a detailed tour de force of both basic and challenging cases in veterinary dentistry.
Extraction Site Preservation, Dr. Rocco Mele
Three minute presentation on extraction site preservation, regenerative techniques and membrane protocol in five clinical cases.
Case Studies
- Periomix: Preserving Teeth Rather Than Extracting (Yee, “Reggie”)
- Periomix Case studies: Preserving teeth, Bilateral Mandibular Fracture Repair, Preventing Fractures, Saving Canines (Yee, Woodward, Redman)
- Periomix Case Studies: Rostral Mandibulectomy & Repairing a Symphysis (Mele)
- Periomix Case Studies: Dental Implant & Large Extraction (Periomix + Block + Ossiflex) (Mele)
- Periomix & Membrane Case Studies: Odontoclastic Resorptive lesions, Vertical & Horizontal Bone Loss, Alveolar Osteitis, Deep pocket Periodontal Disease (Mele)
Brochures
References
- Carranza FA, Takei HH, Cochran DL. Reconstructive periodontal surgery. in: Carranza’s Clinical Periodontology, 10th ed. Carranza FA, et al., eds., Saunders Elsevier, St. Louis, Mo., pp. 972-980, 2006.
- Mellonig JT. Freeze-dried bone allografts in periodontal reconstructive surgery. Dent Clin North Am: Reconstructive Periodontics. July 35(3): 505-520, 1991.
- Hall EE, Meffert RM, Hermann JS, Mellonig JT, Cochran DL. Comparison of bioactive glass to demineralized freeze-dried bone allograft in the treatment of intrabony defects around implants in the canine mandible. J Periodontol. May 70(5): 526-535, 1999.
- Meadows CL, Gher ME, Quintero G, Lafferty TA. A comparison of polylactic acid granules and decalcified freeze-dried bone allograft in human periodontal osseous defects. J Periodontol. 64: 103-109, 1993.
- Samartzis D, Shen FH, Matthews DK, Yoon ST, Goldberg EJ, An HS. Comparison of allograft to autograft in multilevel anterior cervical discectomy and fusion with rigid plate fixation. Spine J. Nov-Dec 3(6): 451-9, 2003.
- Piotrowski M, Pankowski R, Luczkiewicz P, Markowicz A. A comparison of the effect of autogenous vs. frozen homogenous grafts on the healing of non-union of forearm bones. Ortop Traumatol Rehabil. 10(2): 146-51, 2008.
- Klugh DO. Equine periodontal disease. Clinical Techniques in Equine Practice. 4(2): 135-147, 2005.
- Mellonig, JT. Bone allografts in periodontal therapy. Clin Orthop Relat Res. Mar (324): 116-125, 1996.
To see more references for use of bone graft in periodontics, click here >>